Cancer of the pancreas
The pancreas is surrounded by many other vital organs in the abdomen and is in very close contact with large blood vessels that are crucial to life. Tumors of the pancreas very often go unnoticed for a long time because their early symptoms are nonspecific, indeterminate, and are attributed to other very common benign conditions, such as gastritis, dyspepsia, gallstone disease, or back pain. The operation required to remove a tumor of the head of the pancreas (“Whipple procedure”) is by far the most technically demanding abdominal operation. Because of all these reasons (late diagnosis at an advanced stage, technically difficult operation for the average surgeon), almost 95% of such tumors are considered unresectable. Of course they may very well be unresectable when they have already given metastases to the liver or elsewhere, but quite often they are considered unresectable even if they are not really. For example, many surgeons consider these tumors unresectable because they are large in size, they are densely attached to large blood vessels, or because they grow inside the duodenum. We have had a long dedicated experience in surgery of the pancreas and we have developed techniques and strategies with which we can safely remove tumors when considered “unresectable”, or transform initially truly unresectable tumors to resectable. Obviously, these techniques and strategies are not unique to our team, but are implemented to several selected tertiary referral centers around the world with a dedicated interest and a proven track record in pancreatic surgery.
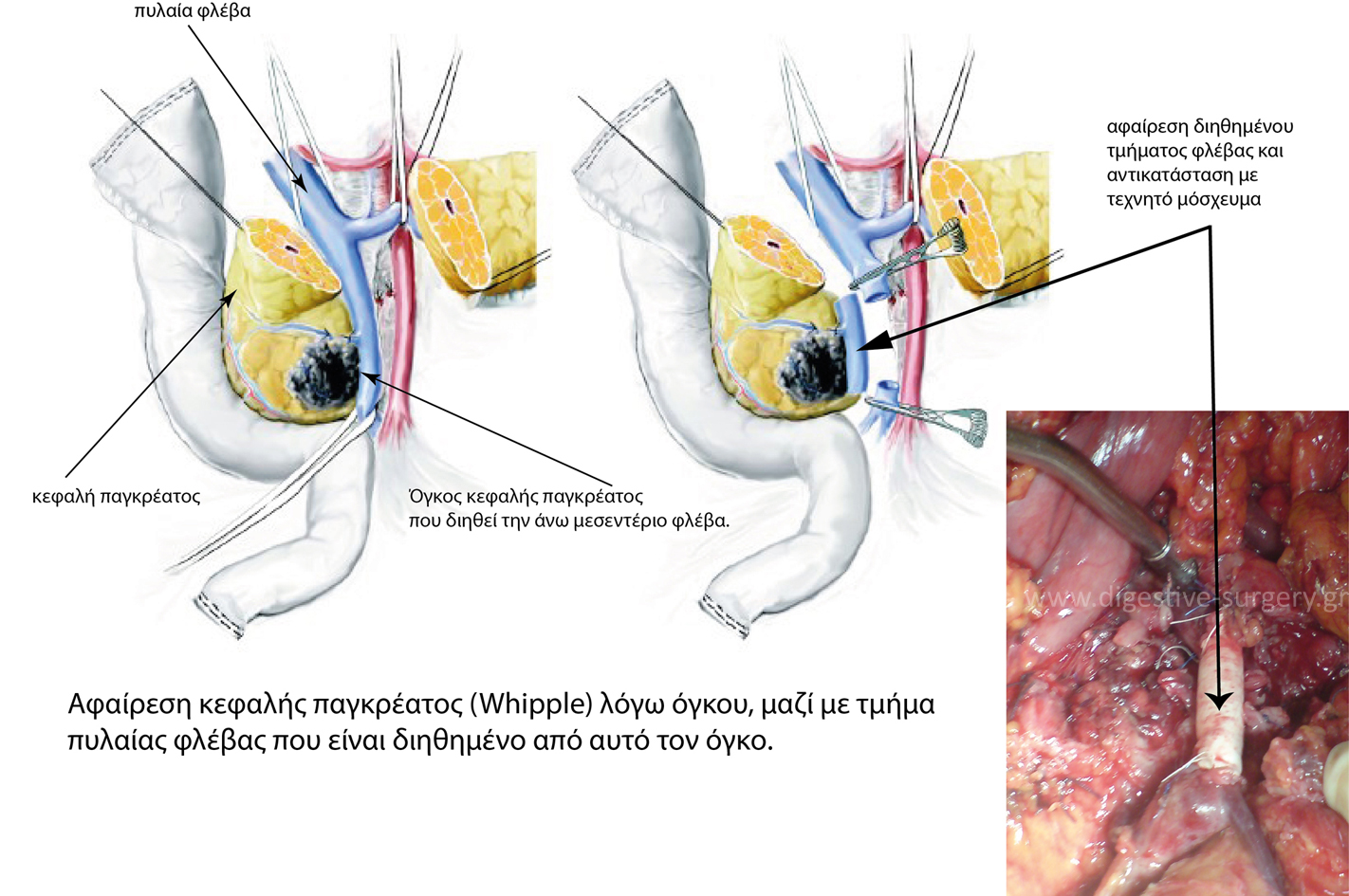
1. When the tumor infiltrates (grows into) the portal vein, or the superior mesenteric vein most surgeons around the world call it “unresectable”. However, this may not be true. One has to study very carefully the CT or the MRI in order to know the exact length of the vessel that is infiltrated, as well as the portion of its perimeter (circumference) involved with tumor. In several cases of vessel infiltration, we have been able to remove the tumor by removing the involved part of the vessel as well, along with the tumor. The resected part of the vessel has then been replaced by a graft, which comes from the same patient, or it may be made of plastic.
2. When the tumor is locally very advanced and infiltrates into larger portions of surrounding vessels and into a wider area around the pancreas (but does not have metastases), we administer neoadjuvant chemotherapy, occasionally associated with radiation therapy. These two regimens may shrink down the tumor (“downstage” it) and convert it to resectable. This way, the tumor “pulls back” from the vessels involved and makes resection possible, usually along with a part of the initially infiltrated vessels.
3. During the operation, we never remove just the part of the pancreas with the tumor in it, but also all the tissue wide around it (fatty tissue and lymph nodes). In order to achieve this, all neighboring vessels are skeletonized (i.e.: stripped of all tissue around them). This is how we are able to perform wide and radical lymph node dissections removing over 15-20 lymph nodes along with the resected part of the pancreas. When the total number of lymph nodes removed is lower than 15, the operation is considered oncologically suboptimal and this may predispose the patient to an early tumor recurrence or early development of metastases.